
Right heart catheterisation is sometimes just shortened to ‘right heart cath’, with the acronym being RHC.
It is a test that assesses the right side of the heart, the side that pumps bloods towards your lungs.
The test doesn’t ‘see’ the right side of your heart pumping like an echocardiogram, and doesn’t look at the blood supply of your heart like an angiogram.
This test is all about measuring pressure – specifically, the test is about looking to see if you have pulmonary hypertension. Sometimes pulmonary hypertension is due to problems with the left side of the heart (most common), sometimes due to issues in the lungs, and sometimes due to a problem with the pulmonary artery itself.
Unlike an angiogram, which involves a catheter going up through your arteries to get to the left side of the heart, a right heart cath involves a catheter going through your veins to get to the right side of the heart.
In terms of putting the catheter in, we can go in through the femoral vein (on either side of your groin), the internal jugular vein (which is in your neck), or the brachial vein (in your arm). Most of the time we will use one of the first two – the last one is technically difficult and sometimes impossible depending on how big the veins are in your arm.
The catheter we use is called a Swan-Ganz catheter, a long, often yellow tube that is passed up into the heart. It has a balloon on it which helps it float through your heart as we take measurements from different places. To see this catheter while it is in your heart, we use low dose X-rays (fluoroscopy). Most of the time, because we aren’t injecting any dye or looking at the heart directly, we don’t save any pictures. The X-ray machine is just to help the catheter go through, and the results are all about the pressure recordings, which can be seen live depicted on a graph.
Usually this procedure is just performed under local anaesthesia, and a very light sedative can be given but the preference is to do it while you are awake so that the most accurate results can be taken (falling asleep or being relaxed can change the pressures in your heart).
The procedure:
- An antiseptic (cleaning) solution is applied to the area. You might feel a cold wash. After this, it’s very important not to move as we need to keep the equipment and your skin sterile.
- You will be covered with a drape – if the procedure is from your neck, this drape may cover your face and often this will be lifted slightly so you can breathe more easily. Be aware it can be slightly claustrophobic.
- Local anaesthetic is inserted into area with a very small needle. You’ll feel a sharp sting initially when the needle goes in, and then a little more stinging as the local anaesthetic goes in. From this point forwards, you shouldn’t feel anything sharp, just firm pressure.
- The sheath is then inserted – this is a small tube that stays in the vein throughout the procedure and acts as a one way valve to let the catheter go through to your heart without causing any bleeding. Sometimes this is done with an ultrasound probe so the doctor can see the vein directly when they put the needle in. When they put this tube in, you will feel them pushing but it shouldn’t be sharp or painful. After this bit is done, the most uncomfortable part is over.
- The catheter will be set up – there may be a pause in the procedure either before or after the sheath goes in, while the team are setting up equipment around you. Don’t be alarmed.
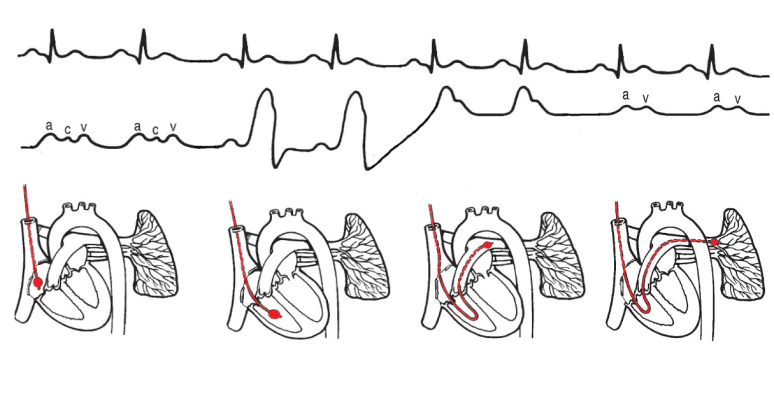
- Using a low dose X-ray machine (fluoroscopy), the catheter is guided towards your heart – first into the top part of the right heart (right atrium), then the lower part of the right heart (right ventricle), then into the tube going to the lungs (pulmonary artery), and finally into the tiny vessels of the lungs (pulmonary capillaries). During this time, you will hear the doctor, technician or nurse calling out various numbers related to pressures within your heart. To take these measures accurately, it is best done with your lungs empty – they may ask you to breathe out and hold your breath out briefly to take each measurement.
- After these measurements are done, they may take a blood sample (mixed venous blood gas), and then measure the flow of blood through your heart (cardiac output). They do this with a series of injections.
- At this stage, the test is done. On average, the measurements themselves take about 15-20 minutes, but the set up before and after can take another 20 minutes.
- The doctor will remove the sheath and press firmly on the area for a few minutes to prevent it bleeding. This may be longer if you are on blood thinners.
- The results of the test are immediately available, and your doctor may discuss them with you there or send them to the person who referred you to have the test done.
Key points:
- Often we’ll get your top half changed into a patient gown if we’re using the arm or neck – if the groin is to be used, then the lower clothes will be removed as well and you will be covered with a blanket.
- You usually don’t have to fast for the test, but check with the hospital performing your procedure.
- You can usually go home on the same day, often after observation for one hour.
- You may have to lie flat for an hour after the procedure if it was done from the groin; if it was from the arm or the neck you can sit up immediately (and often you’ll be sent back to the recovery area in a wheelchair rather than a bed).
- Because they may go through the neck approach, try and remove anything that might be in the area – earrings, necklaces, and tie up long hair. For men, shaving your beard if it is thick on your neck will help.
- If they go through your arm, avoid any strenuous activity or heavy lifting for the next 24 hours.

2 thoughts on “What is right heart catheterisation?”